Kawasaki disease
Kawasaki disease, which affects mainly children, has gotten a lot of attention recently due to the COVID-19 pandemic and the mysterious syndrome which allegedly occurs after resolution of the initial infection (called PIMS, read more here).
But the truth is that is it not a common diagnosis. It is one of the few diseases in pediatrics (which is a very permissive and conservative medical profession), that you cannot miss, so raising awareness may help, regardless of COVID-19.
Who discovered Kawasaki disease and when?
A Japanese physician called Tomisaku Kawasaki described the disease in Japanese in 1967. The disease is called Kawasaki disease after his name.
What is Kawasaki disease?
Kawasaki disease is an example of vasculitis, meaning an inflammation of the blood vessels. In this disease, it is typical for medium size arteries to be effected, mainly those who supply the needs of the heart itself (coronary vessels). It is the most common cause for acquired heart disease in children, in modern countries.
What causes Kawasaki disease?
Practically – unknown. Probably an early infection with an infectious pathogen or an environmental factor that causes inflammation, in children with the right genetic background. It is unclear what is that genetic background, but it is known that although this is a rare condition, the risk of developing Kawasaki disease is 10 times higher in siblings of a patient with Kawasaki.
Who are the patients who are prone to get Kawasaki disease?
First off all children, mainly less than 5 years old. The disease is rare after 8 years old, but there are case reports. Prevalence of the disease in boys is 50% more than in girls.
Ethnicity wise, the prevalence of the disease is different between countries and different ethnic groups. In Asians the prevalence is the highest.
What are the signs and symptoms of Kawasaki?
There aren’t many diseases in medicine which are in fact a list of criteria, but Kawasaki is one of them:
A must have criterion – fever, at least for 5 days.
In addition, 4 out of these 5 criteria –
1- Bilateral nonsuppurative conjunctivitis. This means red eyes without any discharge.
2- Changes of the mucous membranes, which include redness in the throat, dry cracked lips, red lips, and “strawberry” tongue.
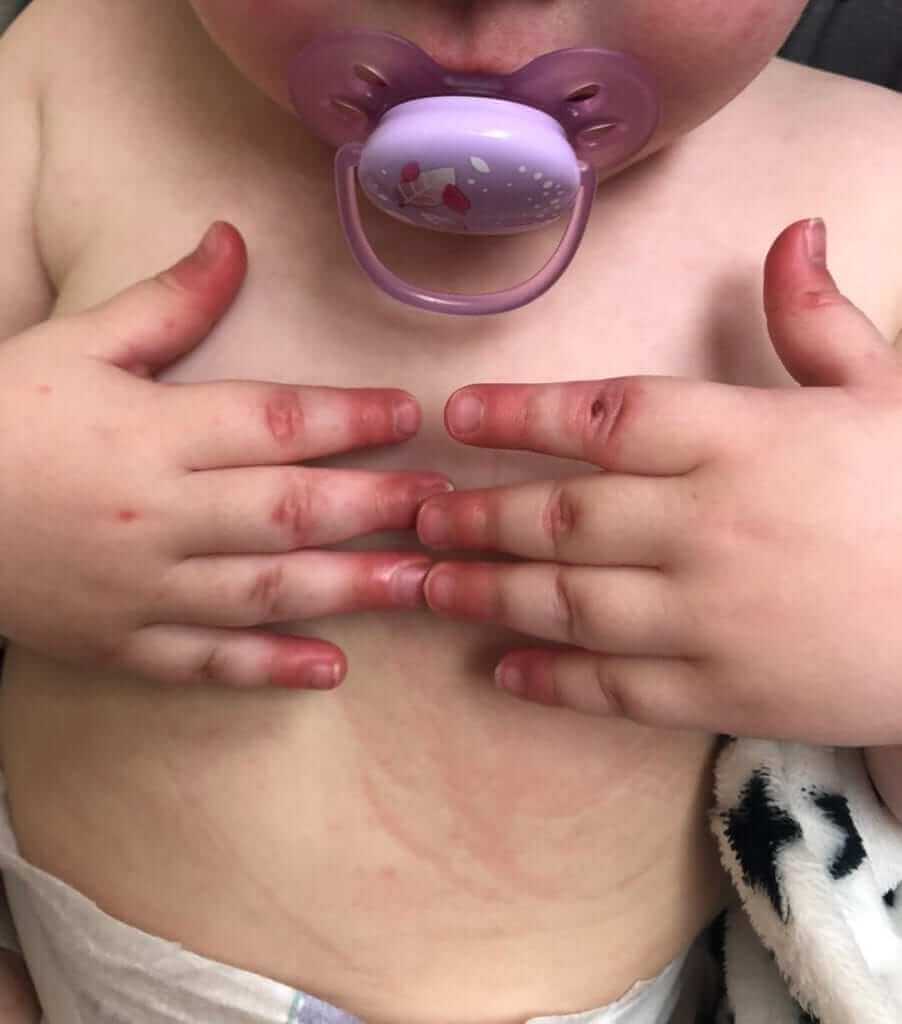
3- Any type of rash, mostly diffuse with accentuation in the inguinal and diaper area. See the adjacent photo.
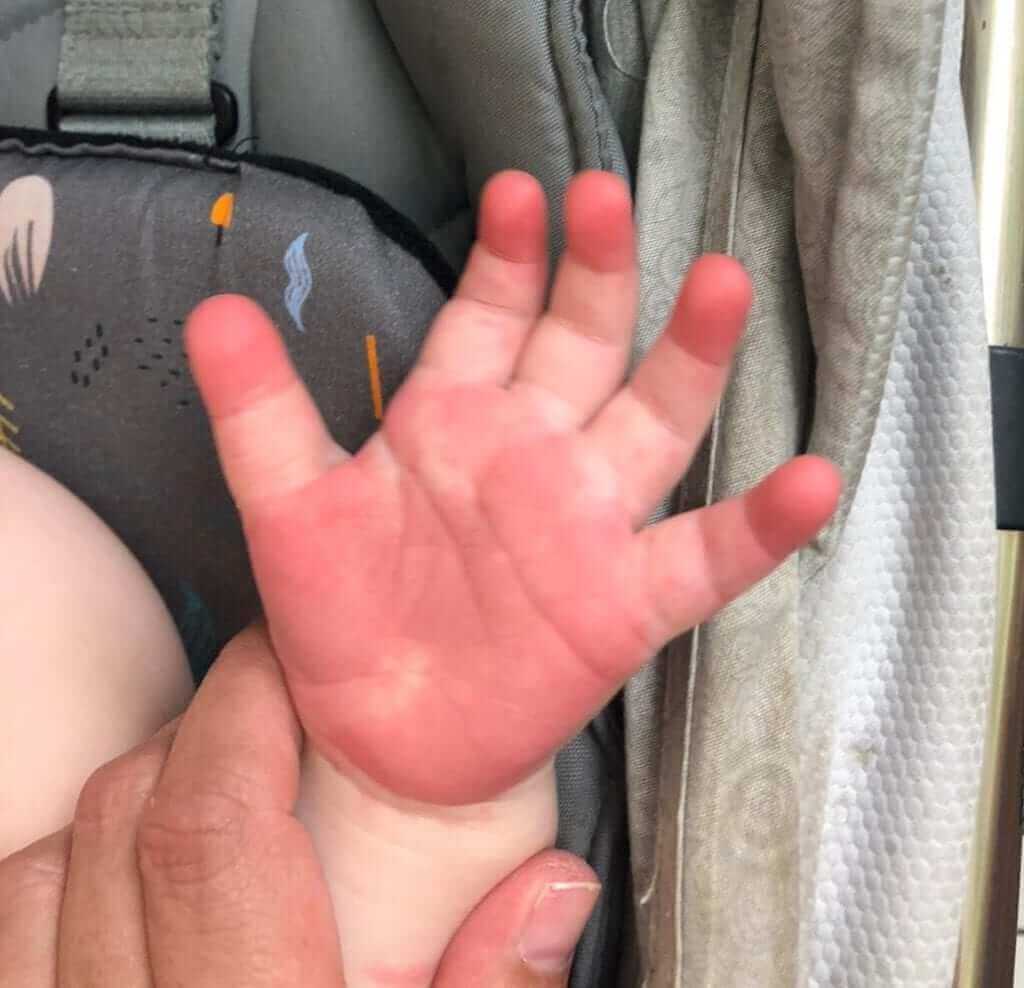
4- Changes of the arms and legs, including redness and swelling. See the adjacent photo.
5- Cervical lymph nodes enlargement, usually one lymph node, unilateral, larger than 1.5 cm in size.
What is typical or complete Kawasaki? A child with a 5 day fever and 4 out of 5 criteria. In some cases, the diagnosis can be made before there are full 5 days of fever.
What is atypical Kawasaki? A child with a 5 day fever, which does not have 4 criteria. Small babies, especially younger than 6 months will most probably display an atypical presentation.
Are there are any more signs besides the classic criteria in a child with Kawasaki?
There are descriptions of involvement of every organ and system in the body in Kawasaki disease, even if it is not listed in the 5 criteria mentioned above.
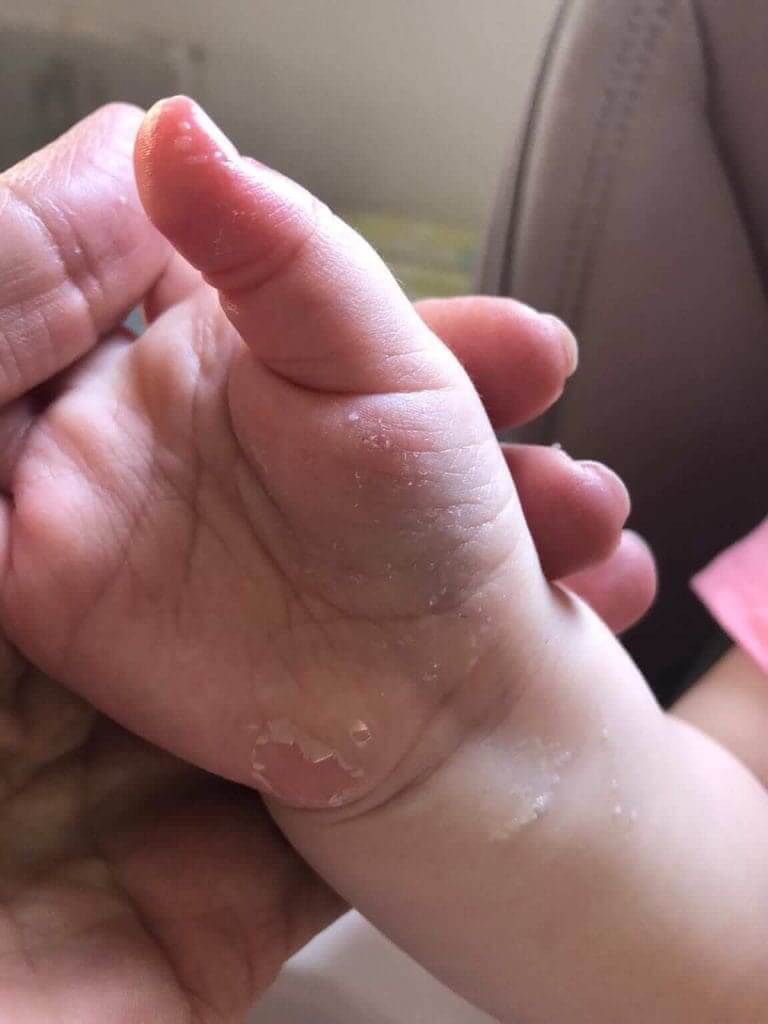
Irritability (restlessness) is very common, sometimes disproportionate to the fever. Gastrointestinal system involvement is also common, manifested as abdominal pain, diarrhea and vomiting. In addition – arthralgia, runny nose, cough, tachycardia and more. Typically, in the second phase of the disease after 10-14 days, there will desquamation of the skin around the nails and the fingers.
What are the typical findings in blood tests in children with Kawasaki?
Unfortunately, every aspect of blood tests in Kawasaki can be affected. The common finding is elevated inflammatory markers, and leukocytes in a urine sample.
So is it easy or difficult to diagnose (or miss) Kawasaki disease?
Not every child will “follow the instructions written in the book” and present with the classical signs and symptoms, making it easier for the physician to diagnose. The experienced physician needs to be aware of this possibility, look for clues during anamnesis, do a thorough physical examination and choose blood tests wisely.
In children younger than 1 year old and older than 5 years old the diagnosis is especially tricky.
Why is there an importance in early diagnosis? What are the risks in Kawasaki disease?
Kawasaki is a disease that would pass on its own, with or without treatment, meaning the inflammation will subside and the child will get better. But! In a child which did not received treatment, there can be cardiac involvement, that would manifest as aneurysms in the coronary arteries, supplying blood to the heart muscle (in up to 25% of cases). These aneurysms can have a long term effect on the child’s health.
Therefore, Kawasaki is a diagnosis that cannot be missed in pediatrics, since early and correct diagnosis (in the first 10 days of fever) lowers the chance for cardiac involvement.
Again, the goal is to diagnose and treat during the first 10 days, not after.
How do you look for cardiac involvement in these children?
By preforming echocardiogram, a non-invasive test with no radiation at all. The test needs to be done under good conditions, when the child is relaxed, which will ensure a thorough examination. Not all findings in echocardiogram are conclusive, and there is a need for close attention and extensive knowledge when preforming the examination. An experienced pediatric cardiologist can identify clues for cardiac involvement even before they reach a state of aneurysm.
What is the treatment for children with Kawasaki?
Besides supportive care, the specific treatment for Kawasaki is a combination of two medications.
Immunoglobulins (IVIG) – mostly in the dosage of 2 grams per kilogram. This is chemical preparation comprised of IgG (Immunoglobulin G) taken from a plasma donation of over 1000 people which contains antibodies against many pathogens.
Anti-inflammatory (high dose) aspirin at first, and then at lower dose for 6 weeks.
In those who’s fever and inflammatory markers will not subside, or in cases where they decrease and then became elevated again, there is a need for consultation with an expert about second line treatment.
What are the long term consequences of resolved Kawasaki?
In a child with no cardiac involvement, there should not be any long term sequela. There is a need to perform an echocardiogram a year after recovery for follow-up. Recurrence of the disease has been described in only a low percentage of cases.
A child with cardiac involvement needs to be in a long term cardiac and rheumatologic surveillance. In these cases you need to differentiate between a mild involvement of the coronary arteries which will pass away and will not leave any damage, to a more sever involvement (aneurysm) than may never pass.
What are the more specific recommendations for a child who had Kawasaki disease?
There are several recommendations in these children –
1- Postpone administration of any live-attenuated vaccine (measles, mumps, rubella and varicella) to 11 months after receiving IVIG in the dosage given in Kawasaki.
2- In children who needs long term treatment with aspirin, a special attention must be given to administration of varicella and influenza vaccine. There is a connection between these infections and a rare syndrome of liver failure in patients under aspirin treatment. A flu vaccine is also recommended for the family of the child who had Kawasaki and is now treated with aspirin.
3- The last recommendation (which is true to all children) is to maintain a healthy lifestyle, to prevent cardiac morbidity. This includes a balanced diet, physical activity, preventing smoking and regular tests for triglycerides in the blood.
Is Kawasaki disease infectious and when can a child be back to his kindergarten?
Though the trigger is probably infectious, it is an inflammatory disease, and therefor is not contagious. The child can go back to his regular activity as soon as he feels better and has normal values of his inflammatory markers (as long as there is no cardiac involvement). In cases of cardiac involvement, a specialist needs to be consulted before returning to every day activity.
What about COVID-19 and Kawasaki?
There are cases of Kawasaki in children who had COVID-19 infection. Some of the cases are with the classic signs and symptoms, and some are not. Many of these children were treated as they would in Kawasaki disease. This outbreak, which was described in the past in regards of other pathogens, just reminds us that there are many triggers to this disease – In this case – the new COVID-19 virus, which can cause Kawasaki disease.
A few words for conclusion:
What should parents do if their child has a 3 day fever? Should they be worried about Kawasaki? Off course not.
They should go get a good medical evaluation, tell their physician the whole story and think together if this is a viral infection (most cases), bacterial infection (the minority of cases) or a different disease such as Kawasaki (rare).
Though Kawasaki is a rare disease most of us will never hear of again, if there is just one child who will get his diagnosis using this website, then I will be happy and ready for early retirement.
For comments and questions, please register
