Oral thrush (oral candidiasis) in children
Oral candida infection, mostly in infants, is a common issue in pediatrics, that makes many parents uneasy, usually unjustifiably…
Do note that this chapter does not cover candida of the buttocks that is part of the bigger topic of diaper rash in children, and certainly not candida infection of other parts of the body, only oral candida, or – ‘oral thrush’.
So what is candida and how did it get to the child’s mouth?
Candida is a common fungus that lives on our skin and in our mouth and pharynx. There are many types of candida, but at this stage the different types are not important.
This mean that it’s not such a special trick to end up with candida in one’s mouth. Both myself and yourselves have candida in our mouth and pharynx this very moment.
But in some cases, as you’ll see later, the amount of candida may increase and cause the child discomfort.
What is the prevalence of oral thrush (oral candidiasis) and what are the risk factors?
An obvious infection of the oral cavity is seen in 2-5% of healthy babies and may develop as soon as a week after birth.
On the other hand, some clear and common risk factors exist for candida over-growth in the oral cavity. Among them are:
Antibiotic treatment – many women are familiar with this issue, of appearance of vaginal candida after treatment with antibiotics for whatever cause. The same occurs with children who receive antibiotics, the natural balance of the oral flora (all the bacteria and fungi that normally live together in peace and comradery), in disrupted, and the candida “rears its head” and thrives.
The use of inhalations or nebulizers – using inhalation/nebulizers is a risk factor for oral thrush. An excellent way to avoid this is by washing the mouth or drinking something after every treatment.
Throat infection – normally, we produce saliva and swallow it, and the abundance of oral bacteria and fungi live in peace. When children have a throat infection and they don’t swallow their saliva and the candida may thrive. I see this mainly after herpes infections of the oral cavity, but it may be seen in any illness that causes pain when swallowing and the child avoids food or drink.
Obviously, there are other risk factors, mainly immune compromise, and these conditions are sadly associated with children suffering from chronic diseases.
How does oral thrush look like?
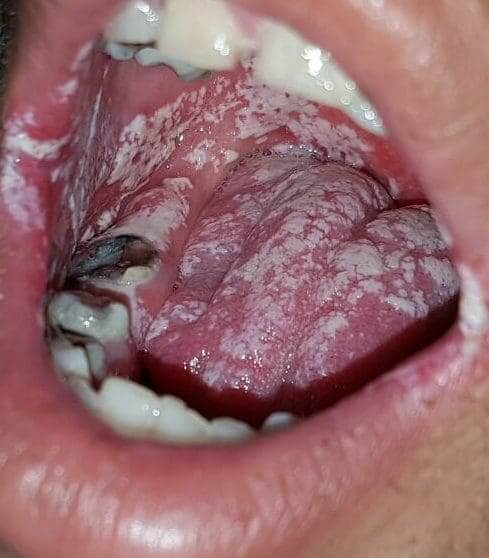
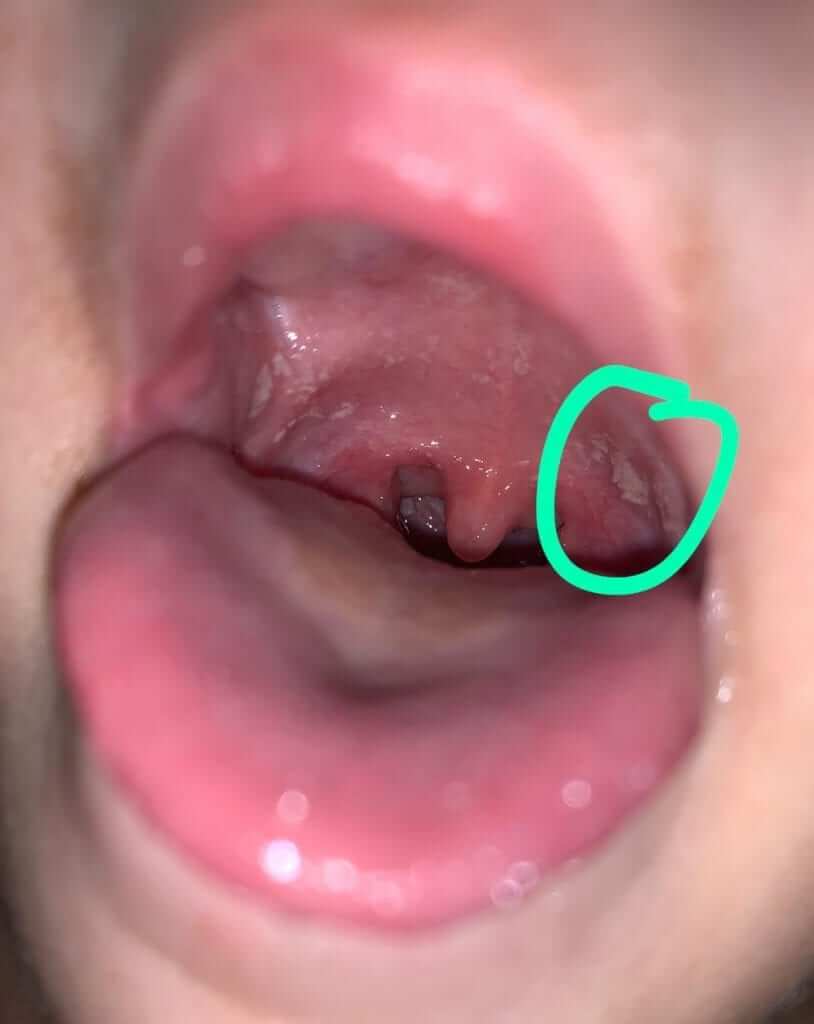
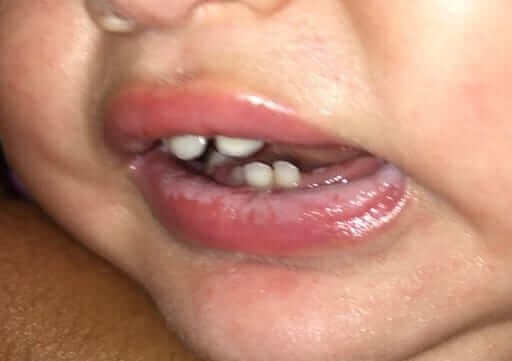
Typical white spots in the pharynx, palate, tongue and sometimes lips. A skilled doctor would know how to distinguish between candida and other types of oral infections. The appearance is that of chalk sometimes.
See the three picture attached in this chapter. In the first photo, relatively thick white coating over the tongue, the second is candida in the area of the palate and the third shows candida on the lips.
Are special tests required to diagnose candida?
Absolutely not. Observation of a mother or a skilled doctor will suffice.
Does oral candida necessarily cause clinical manifestations in a child?
Although it’s sometimes hard to know (especially with babies), candida infection will not cause certain symptoms every time.
If there are clinical manifestations, they may include discomfort, pain, particularly while eating and reduced appetite.
What is the treatment of oral thrush in babies and children?
I will remind you that treatment is not always required. I see many babies with a little bit of candida on their tongue and usually this doesn’t justify treatment. More examples of children for whom I would not recommend treatment:
If the child had already completed the antibiotic treatment and a small amount of candida appears – treatment is not necessarily required. Simply the completion of the antibiotic treatment will allow restoration of the balance in the oral cavity and the candida will cease to thrive.
If the child is already recovering from the throat infection (viral or bacterial) and is eating and drinking again, the candida will usually disappear on its own.
But if there are clear symptoms or if the candida is seen all around the oral cavity, including the palate and the inner cheek, treatment may be considered.
If we wish to treat, these are the principles:
• Stop, if possible, the cause that brought the candida about. Treat the throat infection, reduce unnecessary antibiotic treatment, and wash the mouth after using a nebulizer/inhaler containing steroids.
• Whenever possible, reestablish normal feeding. This is an excellent remedy for candida.
• Local treatment in the oral cavity – there are several preparations that treat candida in the oral cavity. The most practical in my opinion is Micnozole oral gel. The grl should be applied in the child or baby’s oral cavity, a finger may be used. The gel may also be put on the dummy. In breast-fed babies the gel may also be applied on the nipple.
In conclusion, a common condition is pediatrics.
Does not always justify treatment, but does justify acknowledgement and thought and in certain cases, appropriate treatment may be helpful.
Good luck.
For comments and questions, please register
