PFAPA Syndrome in children and adults – recurrent episodes of throat inflammation
PFAPA is a the most common syndrome causing recurrent fever in childhood. Being familiar with this syndrome is important for adequate management and relief of suffering. It is also very important to be able to diagnose this syndrome properly, because this diagnosis is often missed in many children and they end up taking multiple unnecessary courses of antibiotics.
I am aware that despite it being under “infectious diseases” on our website, PFAPA is not an infectious disease but rather an inflammatory/rheumatologic disease. However, since this syndrome imitates a bacterial infection of the throat, I chose to place it both under the infectious diseases section and the rheumatological disease section on this website.
Indeed, this post was written by the disease specialist, Professor Gil Amarilyo, a senior pediatric rheumatologist listed under Dr Efi’s recommended physicians in the following link.
What does PFAPA stand for?
PFAPA is an acronym for:
Periodic Fever – recurrent fever, repetitive episodes of fever at set intervals
Aphthous – in some of the cases there can be aphthous ulcers in the mouth
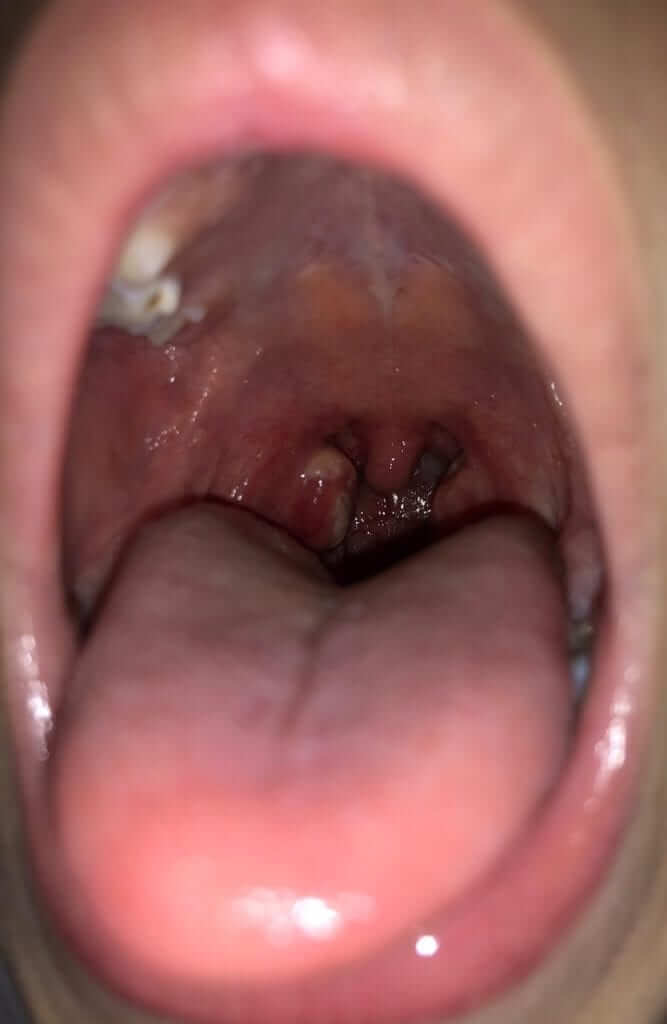
Pharyngitis – tonsillitis with exudates, see image attached
Adenitis – swelling of the lymph nodes in the neck
At what age does PFAPA commonly occur?
PFAPA typically presents at ages 2-5 years, but it can affect all the different age groups, including young adults.
What are the signs and symptoms of PFAPA?
In PFAPA there are recurrent episodes of fever, usually every 3-6 weeks. Sometimes the episodes are even more frequent. What does each episode include? Fever, fatigue, sore throat with exudates (pus) on the tonsils, swollen lymph nodes in the neck region and sometimes sores in the mouth. These signs may be accompanied by headaches, abdominal pain and joint pain.
How long does an episode of PFAPA last without treatment?
It will usually last about 4-6 days (approximately), regardless of antipyretic or antibiotic treatment (the latter is completely unnecessary).
What causes PFAPA? What is the difference between an infection and an inflammation?
PFAPA is an example of an inflammation, not an infection – the immune system is responsible for both of these.
We are all aware that infections can cause inflammation (such as in pneumonia or a urinary tract infection caused by bacteria). But inflammation can also develop without the involvement of bacteria. For example, when a muscle in the back is strained or there is trauma to a muscle – our body responds with inflammation despite the absence of bacteria or viruses. In other words, keep in mind that not every inflammation is caused by an infection.
The trigger for PFAPA is not clear. One possibility is that it is the result of an abnormal reaction to a pathogen, but a pathogen has yet to be discovered. It is also possible that it is not associated with any pathogen at all. But obviously, since it is not caused by bacteria, antibiotic treatment is not helpful.
How is PFAPA diagnosed by the pediatrician?
On the one hand this seems to be an easy diagnosis – recurrent episodes of fever and sore throat that are cyclic in character. There are almost no other syndromes in pediatrics similar to this one. On the other hand, you need to have the opportunity to observe the patient over a period of time to be able to suspect and recognize that they have this syndrome. It is, therefore, very hard to diagnose this on the first or even the second episode.
And thinking retrospectively – are you familiar with those adults that complain of having had recurrent strep throat infections as children? The ones that tell us about how they used to get penicillin injections for their infections and underwent a tonsillectomy because of this? Well, with the benefit of hindsight we can now tell that what they probably had was PFAPA, and not recurrent strep throat infections.
What are the findings on examination of a throat of a child with PFAPA? Should a throat swab be taken?
Every time a child has an episode of PFAPA, they will have tonsils with white exudates. They may not be visible on the first or second day of illness, but they will always appear eventually.
In my opinion, every time a child presents with exudative tonsillitis, a throat swab should be obtained – either a rapid test or culture.
A negative swab raises concern for PFAPA.
When the swab is positive the physician should consider the possibility of a true streptococcal infection that requires antibiotic treatment or a carrier state, found in 15% of the general population.
What should I do if my child has already been diagnosed with PFAPA and he/she has developed a sore throat again? How can I tell whether this is another episode of PFAPA or strep throat?
So, first of all, most parents and children with PFAPA are able to tell whether this is another episode of PFAPA or something else. Despite there not being much of a difference between an episode of PFAPA or strep throat infection, there are still certain signs that the child with PFAPA will have that help their caretaker determine that this is an episode of PFAPA. On the other hand, one must keep in mind that children with PFAPA can also develop strep throat, just like any other child.
Therefore, every time it is unclear whether this is an episode of PFAPA or strep throat, a swab should be obtained. And never forget the possibility of a child being a carrier of strep. You can read more about streptococcal infections in this post.
What happens to a child with strep throat who receives steroidal treatment as needed for PFAPA? Most of the time they will improve for about 12 hours, but the fever will then resume.
What is the treatment for PFAPA?
The treatment for PFAPA is a single dose of steroids that leads to a dramatic improvement in the way the child is feeling.
The dose and type of steroidal treatment recommended depends on the child, their weight and their ability to swallow/take in medication and it is always best determined by a physician who is familiar with the disease.
In most cases, because children with PFAPA are usually young, they will be prescribed soluble steroidal tablets such as betamethasone.
What is the recommended dosage of steroids for the treatment of PFAPA?
It is important to distinguish between the treatment needed for the child’s first episode and the upcoming episodes.
The first time the child is suspected to have PFAPA, the treatment recommended also has a diagnostic significance. The drastic improvement in the child following treatment with steroids, helps confirm the diagnosis. It would be a shame to miss it because of a low dosage of steroids.
Therefore, a child is advised a dosage of 0.2-0.3mg/kg of betamethasone for their first episode of PFAPA. For example, a child that weight 15 kg will need 3-4.5mg, given this is their first episode.
Once the diagnosis has been confirmed, the next episodes can and should be treated with lower doses of steroids. The goal is to give the child the lowest possible dose of steroids that gets the job done (usually through trial and error) and breaks the flare.
What does “breaking the flare” in PFAPA mean?
This means that the episode of PFAPA has subsided, and that the next episode started at least 7 days later. This helps us understand what will happen if we administer lower doses of steroids that do not “break the flare”. The episode will not end and will resume within the following 7 days. This is usually a sign that the dosage of steroids that the child received was insufficient (or that there was a misdiagnosis, and the child is not actually suffering from PFAPA).
Can treatment with higher doses of steroids, whether on single or multiple occasions, be dangerous to the child?
No, a single high-dose of steroids is not dangerous.
Some children can develop irritability as a side effect of treatment with betamethasone. In these children it is important to try and find the balance between the dose of betamethasone that is high enough to “break the flare” but low enough to avoid irritability. If unable to find an appropriate dose, switching to a different steroid that does not cross the blood-brain-barrier should be considered together with the physician.
Except for the unpleasant sick days that the child may suffer from, neither the syndrome nor the treatment affect the child’s growth or development.
Are there other available therapies for PFAPA?
If a child has a case of resistant PFAPA that does not respond to steroids, you should consult with a specialist. There have been attempts at treatment with other medications in these cases, such as cimetidine, montelukast and colchicine and some children respond well to these. In very resistant cases, tonsillectomies are considered.
What happens to children with PFAPA as they grow? When does it go away?
As the child grows, the frequency of the episodes decreases. In most cases, the child eventually “grows out” of the disease. It’s interesting though that in some children the frequency of episodes increases after the diagnosis is made and treatment with steroids is started.
What is extreme PFAPA?
Extreme PFAPA occurs in a subset of children with PFAPA. In extreme PFAPA episodes occur in intervals that are shorter than 2 weeks, for a period of at least 3 consecutive months.
An new scientific study described the characteristics of this condition, and a summary of this study can be found on our website, in the link here.
Is it really worth offering treatment for PFAPA? Afterall, it’s only a few days of fever…
PFAPA is an unpleasant disease for the child, even if it is not dangerous. Having 3-6 days of high fever is not something I wish upon any child…
Therefore, I encourage you not to be afraid of treatment with steroids. The benefits of a single dose of steroids (drastic improvement and the ability to resume regular activities the following day) greatly outweighs the minor risks that steroidal treatment, once every 3-6 weeks, poses.
At the same time, it is worth noting that even if the child does not receive treatment, there will be no harm inflicted upon him/her other than a few sick days.
A few words to wrap it up:
Unfortunately, despite us living at a time where all this medical information is available and accessible (for parents too), many cases of PFAPA are missed by healthcare professionals. Often parents are the ones to bring this up in front of their physician, after reading posts such as this one and drawing the possibility of this diagnosis to the physician’s attention.
It is, indeed, easy to miss this diagnosis during the child’s first or second episode, but when these episodes recur more often, at set periods of times, it is important to consider the possibility of PFAPA.
The syndrome has no long-term effects, and the treatment, even though it can be annoying at times, is simple and leads to full recovery.
For comments and questions, please register
